Crumbling foundations
The impact of failing public services on health and productivity
16 February 2023
6 minute read
Download the report, Crumbling Foundations: the impact of failing public services on health and productivity
New analysis by the Centre for Progressive Policy (CPP) highlights the impact in lost life years and years of good health of socioeconomic inequalities in employment, income, education, crime and housing. It finds that people in England are losing 1.5 years of life and 2.6 years of good health on average because of these factors, which equates to 81 million life years and 144 million years of good health lost across England.
A healthier and more productive society cannot be built on public services that are crumbling into disrepair. To reverse these trends, improving outcomes across these social drivers of health by strengthening public services must be a priority.
CPP's new paper makes the economic case for investment in public services to improve population health, productivity and fiscal sustainability. It will be followed by a paper setting out national policy proposals for reform.
Key findings
- In Sandwell, one of the most income deprived areas, CPP estimates that people will live around 4.4 years fewer, 90% of which can be attributed to these five factors: higher levels of unemployment (0.7 years), lower income (0.8 years), educational disadvantage (1.9 years), higher risk of local crime (0.4 years) and poorer quality housing (0.3 years).
- In the most deprived areas people are living several years less: 6.4 years in Blackpool, 5.5 years in Manchester, 4.9 years in Knowsley and 5.3 years in Liverpool. The analysis estimates the impact of socio-economic inequalities on these differences but cannot explain them in full, highlighting the importance of local data to understand the full picture.
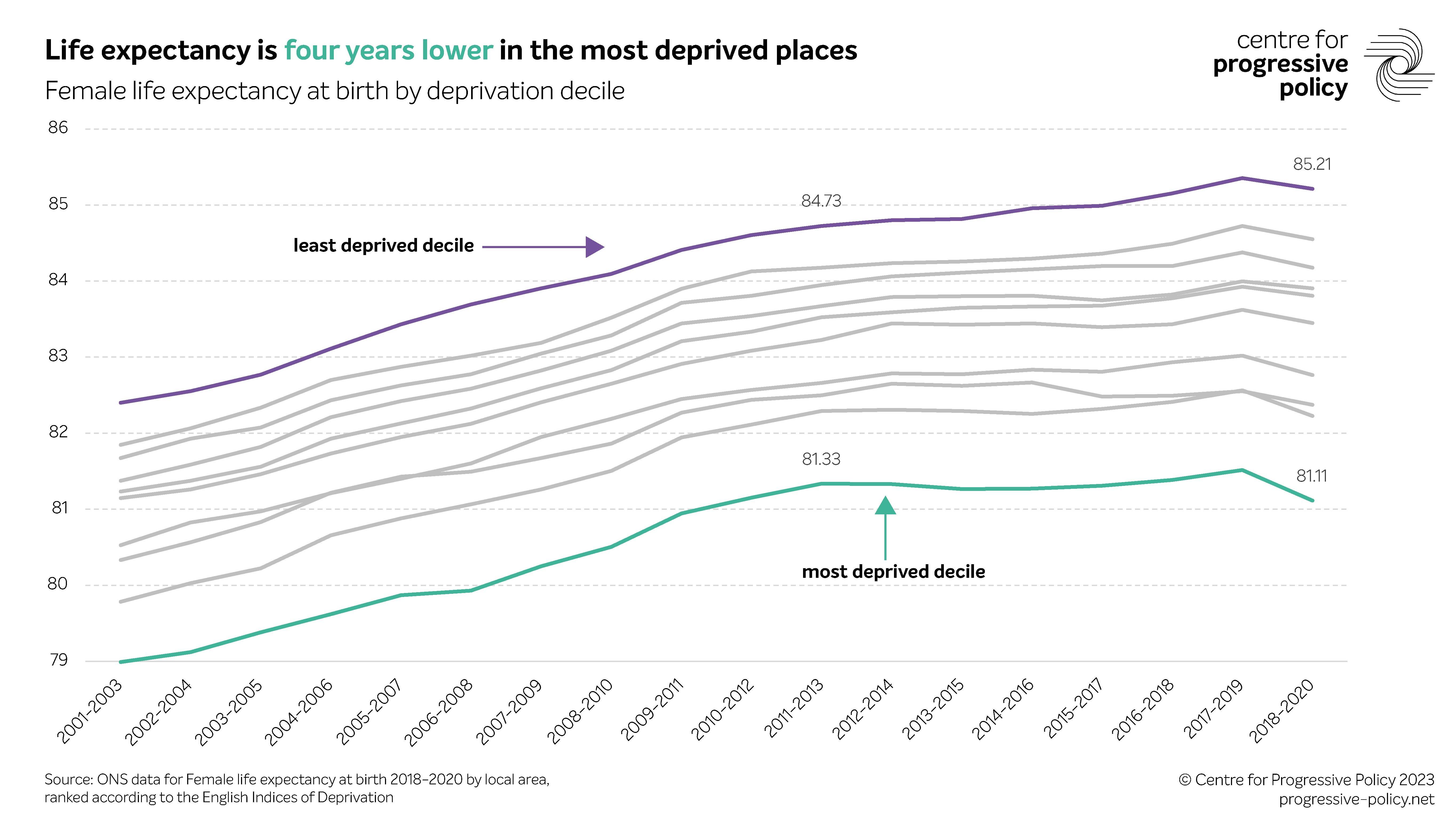
These socioeconomic factors are driving alarming disparities between
the number of years people in England can expect to live in different places. For the most deprived local authorities in England, female life expectancy is over four years less than in the least deprived.
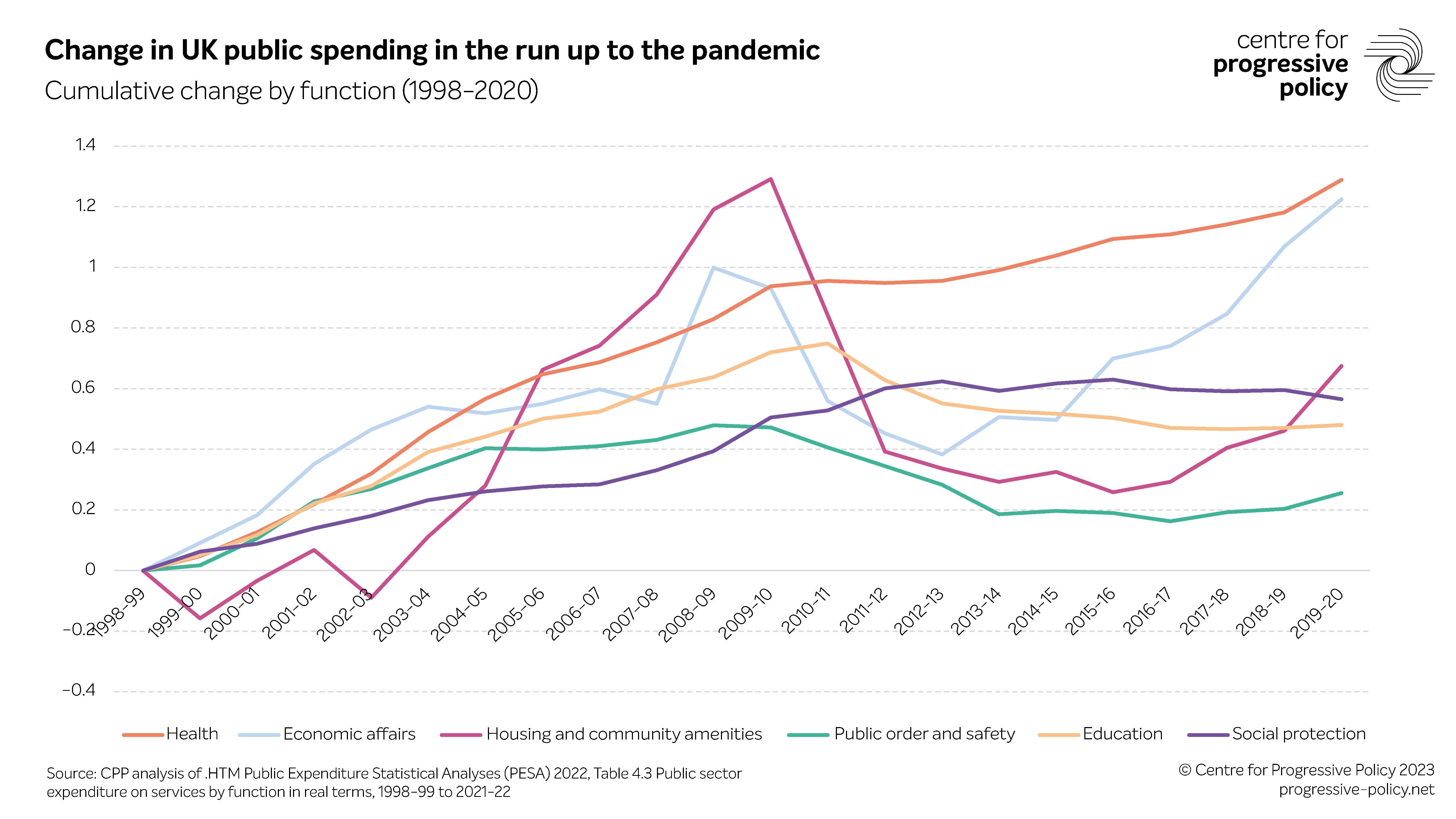
With record high levels of economic inactivity, poor health preventing people from re-entering the labour market and the retirement age set to rise to 68 despite stagnating healthy life expectancy, improving people’s health must be a priority. To do so, governments must look outside the healthcare system. Previous CPP analysis of OECD countries shows that countries that have increased spending on social protection such as unemployment support and education have experienced improvements in life expectancy.
This model specifically focuses on non-health factors because despite healthcare being one of the only areas of spending protected by the UK government since 2010, the UK’s health outcomes are not improving. The social determinants of health – income, employment, education, housing and crime – have the greatest influence on ill health and yet they are chronically undervalued. Overall, relative levels of educational disadvantage between places are the strongest socio-economic predictor of life expectancy for both men and women.
The healthcare system is on an unsustainable footing, with a rapid growth in hospital admissions, mass exodus of staff, and inability to weather shocks like the Covid-19 pandemic. The UK is the only developed country where the proportion of working-age people not employed or seeking work has continued to rise since the height of the pandemic. A long-term build up in poor population health is contributing to these issues, increasing A&E admissions and preventing people from re-entering the labour market.
The link between social determinants and locally designed and delivered public services is crucial: a healthy, productive society cannot be built on crumbling public services and hollowed out local infrastructure. Spending must be reformed to enable investment in preventative public services, determined and delivered by local leaders, to achieve the transformation in educational outcomes, employment and earnings that is needed.
Rosie Fogden, Head of Research & Analysis at CPP said:
“Poor health is doing profound harm to the wellbeing and productivity of the UK population, and our analysis shows that varying levels education, employment and income deprivation can explain much of the difference in life expectancy between local areas.
“We cannot afford to continue to neglect preventative public services like children’s services, adult education and housing support services as they crumble, and then increase health spending to deal with the consequences later down the line.
“Improving people’s health through effective, locally tailored public services like skills training and mental health support must be a priority if we are to shift onto more productive track and bring down national healthcare spending in the long term.
“Bold action today has the potential to reduce simultaneously the pressure on future services and generate productivity and economic growth for the benefit of people and communities.”
Commenting on CPP's findings, Lisa Nandy MP, Shadow Levelling Up Secretary, said:
“It is unconscionable that so many of our communities continue to suffer from stark health inequalities, despite the Conservatives making narrowing such inequalities a central goal of ‘levelling up’. After Covid, when communities in the North were locked down for far longer than other parts of the country, tackling the problem is even more vital.
“Labour will launch the biggest expansion of medical training in history, giving the NHS the staff it needs in every part of the country, paid for by abolishing non-dom tax status. But these inequalities are deep-rooted and it will take a cross-government approach where we stop writing off huge swathes of the country and the contribution they have to make.”
CPP will publish further research setting out policy recommendations as to how to achieve this in the spring.
Notes
Estimates of life years lost are based on a comparison with average life expectancy at birth in the 10% least deprived local authorities.
CPP have then modelled how many years of life are lost in different places compared to this standard because of five socio-economic outcomes: unemployment, income, educational disadvantage, risk of local crime and poor housing quality.
The analysis is based on the 2019 English Indices of Multiple Deprivation and ONS life expectancy and healthy life expectancy data for 2016-2018, alongside data on unemployment and household income. The model explains 80% of local variation in life expectancy and 60% of the local variation in good health across England. As a cross sectional analysis, it cannot be said to demonstrate causality between the social determinants of health and life expectancy.
This updates previous CPP work for the Beyond the NHS report, published in 2019. For methodological details see: https://www.progressive-policy...;